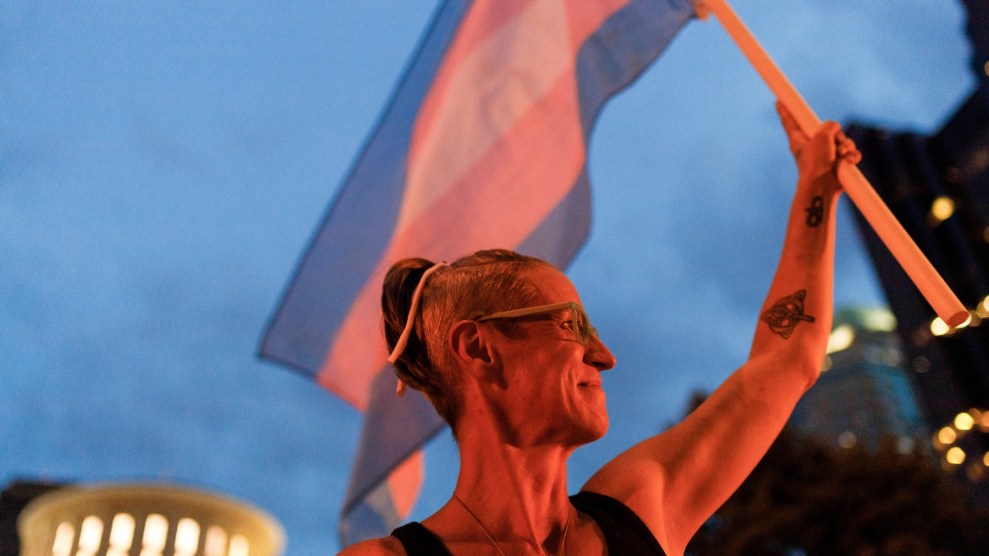An oil refinery in Plaquemines Parish, Louisiana. New research indicates that industrial air pollution may explain the disproportionate rate of coronavirus deaths in the state’s chemical corridor. VW Pics via ZUMA Wire
This story was published originally by ProPublica, a nonprofit newsroom that investigates abuses of power. Sign up for ProPublica’s Big Story newsletter to receive stories like this one in your inbox as soon as they are published.
The industrial plants in the riverside Louisiana city of Port Allen have worried Diana LeBlanc since her children were young. In 1978, an explosion at the nearby Placid oil refinery forced her family to evacuate. “We had to leave in the middle of the night with two babies,” said LeBlanc, now 70. “I always had to be on the alert.”
LeBlanc worried an industrial accident would endanger her family. But she now thinks the threat was more insidious. LeBlanc, who has asthma, believes the symptoms she experienced while sick with the coronavirus were made worse by decades of breathing in toxic air pollution.
“That is the one time in my life I thought, I’m not going to survive this,” she said. “I’m going to become a statistic. I was that sick.”
New research, conducted in part by ProPublica, shows she could well be right.
COVID-19 can be made more serious—and, in some cases, more deadly—by a specific type of industrial emission called hazardous air pollutants, or HAPs, according to new peer-reviewed research by ProPublica and researchers at the State University of New York College of Environmental Science and Forestry. The study, published Friday in the journal Environmental Research Letters, found this association in both rural counties in Louisiana and highly populated communities in New York.
The analysis examined air pollution and coronavirus deaths in the roughly 3,100 U.S. counties and found a close correlation between levels of hazardous pollutants and the per-capita death rate from COVID-19.
The U.S. Environmental Protection Agency defines HAPs as chemicals known or suspected to cause cancer and other serious health problems. Under the Clean Air Act, industrial facilities emitting these pollutants are subject to regulations.
Hazardous air pollution may help explain the disproportionate number of COVID-19 deaths in communities like West Baton Rouge Parish, home to Port Allen. With 39 deaths as of Sept. 7, the parish’s per-capita death rate from COVID-19 ranked it among the top 3% of all U.S. counties with at least 30 deaths. Several of its neighbors in Louisiana’s industrial corridor also rank near the top of the list.
COVID-19 and Air Pollution Exposure
The coronavirus pandemic, which has claimed over 189,000 lives across the country, including more than 4,900 in Louisiana, offers a rare opportunity to study the public health outcomes of both short- and long-term air pollution exposure.
Because the virus affects the respiratory system, researchers have rushed to study the potential association between mortality rates and air pollution. Early studies, including one looking at particulate matter—distinct from HAPs, but often found with them—have suggested a link.
Last year, the Times-Picayune and the Advocate and ProPublica published the series Polluter’s Paradise, which used data from an EPA model to quantify levels of hazardous air pollution along the lower Mississippi River’s industrial corridor. As the virus battered many of those same communities this spring, we wanted to determine whether air quality was contributing to high death rates.
The SUNY-ProPublica analysis uses pollution information from the EPA’s 2014 National Air Toxics Assessment, a screening tool aimed at helping state agencies identify and measure the sources of HAPs. These pollutants can come from industrial facilities as well as from power plants and vehicles.
NATA combines information on pollutants that affect the respiratory system into a variable called the “respiratory hazard index.” The analysis found that an increase in the hazard index at the county level corresponded to an increase in COVID-19 death rates. This association existed at all levels of HAPs exposure, including levels that the EPA deems acceptable.
The analysis controlled for a long list of variables, including population density, income, race and age, as well as community health indicators such as prevalence of smokers, adult obesity, preventable hospital stays and physical inactivity.
Peer Review
A recent study by researchers from Harvard’s T.H. Chan School of Public Health found that long-term exposure to particulate matter made the coronavirus more deadly. But EPA officials and industry groups have dismissed the research primarily on the basis that it lacks peer review, a standard but time-consuming process where new research is evaluated by independent experts prior to publication.
ProPublica and the Times-Picayune and the Advocate sent the EPA a copy of the new analysis on hazardous air pollutants, which has been peer reviewed, seeking comments. Enesta Jones, a spokeswoman for the agency, said that understanding the links between air pollution and COVID-19 is a “complicated process that will take many years.”
“The research in this area is just beginning, and EPA looks forward to reviewing papers once they are peer-reviewed and published,” she said.
Cancer Alley
The industrial corridor that stretches alongside the Mississippi River from Baton Rouge to New Orleans is nicknamed “Cancer Alley” because of the perceived health risks associated with local chemical emissions. LeBlanc considered herself lucky because no one in her family has had cancer. But she does have asthma, and so do two of her three children.
According to EPA data, West Baton Rouge Parish has more air pollution that affects the respiratory system than 99% of counties nationwide.
Research has long supported an association between asthma and exposure to air pollution. While researchers are not sure how this happens, they believe air pollutants could prevent the body’s immune system from being able to tell the difference between a harmless allergen and a dangerous particle, like a virus. The U.S. Centers for Disease Control and Prevention has said that people with asthma are at higher risk of getting very sick from COVID-19.
In mid-March, LeBlanc began having flu-like symptoms. It started as a fever and cough. “Then, the second week it got doubly worse,” she said. LeBlanc went to a drive-thru site in Baton Rouge to get tested for coronavirus. Her test came back positive.
She was sicker than she’d ever been. “I had nightmares. I had coughing. I had aches in my bones. I couldn’t even touch myself,” she said. “That’s how painful it was.”
LeBlanc has nearly recovered. But she said she still has not regained her senses of smell and taste and she gets fatigued more quickly. She believes her debilitating symptoms owed partly to her compromised immune system. “Now what causes your immune system to be down? Is it the air you’re breathing?” she asked.

Diana LeBlanc and her son David at her home in Port Allen, Louisiana. Diana, David and her other two children all have asthma.
David Grunfeld/The Times-Picayune and The Advocate
Dr. Michael Brauer, a professor of public health at the University of British Columbia, said there is substantial evidence of a link between air pollution and respiratory infections. “If you’re exposed to a viral infection or bacterial infection and at the same time are exposed to air pollution, that infection is more likely to become severe,” he said.
But air pollution can also have permanent effects on health that make COVID-19 symptoms more severe, whether or not a person continues to breathe in polluted air. Vijay Limaye, an environmental health scientist with the Natural Resources Defense Council’s Science Center, said that short-term declines in air pollutants in New York City due to lockdown measures in March and April did little to protect populations suffering from long-term exposure.
“In some cases, damage to our lungs, our brains, our hearts from air pollution is irreversible. And there are certain harms inflicted by these exposures that can’t be mitigated even after months or years of breathing cleaner air,” said Limaye.
Asthma Alley
ProPublica and SUNY researchers created a nationwide ranking of counties by combining two variables: COVID-19 mortality rate and the quantity of pollution affecting the respiratory system. First on the list is the Bronx, a borough that was hit particularly hard by COVID-19.
“The air quality issues here and the type of decision-making that’s happened over and over has made us Asthma Alley,” said Mychal Johnson, an organizer from the South Bronx, referencing the local nickname of an area with one of the highest asthma hospitalization rates in the country.
“Waste transfer stations, fossil fuel power plants, heavy diesel trucking,” Johnson said, listing the various sources of pollution in the South Bronx. “We knew that what we had been fighting all these years was only going to make us more susceptible to COVID mortality.”
While all of New York City’s five boroughs except Staten Island occupied slots in the study ranking’s top 20, the remainder of the list included more sparsely populated counties in Louisiana, Alabama and Georgia that contain industrial facilities or power plants. Five counties in the top 20 are located on the lower Mississippi River in Louisiana’s chemical corridor, including West Baton Rouge Parish.
LeBlanc’s son moved his family to a farm farther away from chemical plants in the parish because of his concern about air pollution, and his mother is moving there soon. But a trucking company just north of the property is seeking a permit from the state to increase its air pollution.
“I do worry about my grandchildren,” she said. One of her grandsons has severe asthma and allergies, at times requiring a nebulizer. “It’s just something we’ve had to live with, and that’s the terror of it,” she said.
When LeBlanc’s children were young she had a bag packed at all times in case an industrial accident happened and they needed to evacuate. “I lived in fear of just having to pick up my babies and run,” she said. “I did everything I could for them and here it’s come to the next generation.”