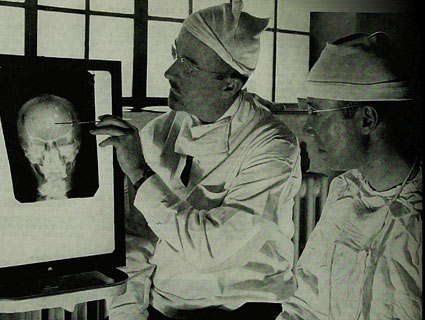
Between 2009 and 2012, states cut a total of $4.35 billion in public mental-health spending from their budgets. According to a report by the National Alliance on Mental Illness, significant cuts to general fund appropriations for state mental health agencies have translated into a severe shortage of services, including housing, community-based treatment and access to psychiatric medications. “Increasingly, emergency rooms, homeless shelters and jails are struggling with the effects of people falling through the cracks,” the report says, “due to lack of needed mental health services and supports.”
The map below shows how states’ spending changed on mental health services between 2009 and 2012. Click on a state to see the specifics.

These six states and the District of Columbia made the deepest cuts to their mental health budgets.
South Carolina ($187.3 million in 2009 to $113.7 million in 2012, -39.3 percent): The director of the local NAMI chapter says the state’s mental-health department is “approaching crisis mode with funding at 1987 levels.” After closing community mental-health centers and reducing services at its remaining facilities, the department is now serving thousands fewer patients.
Alabama ($100.3 million in 2009 to $64.2 million in 2012, -36 percent): Alabama has one of the lowest numbers of psychiatrists [PDF] per capita in the nation. Despite rising demand for psychiatric hospital beds, Alabama plans to close most of its state mental hospitals this spring, laying off 948 employees.
Alaska ($125.6 million in 2009 to $84.7 million in 2012, -32.6 percent): Alaska has the nation’s No. 2 suicide rate—and a massive mental-health workforce shortage. Sometimes there is not a single psychiatrist or psychiatric nurse [PDF] available at the mental-health center in Fairbanks, the state’s second-largest city.
Illinois ($590.7 million in 2009 to $403.7 million in 2012, $-31.7 percent): Illinois has more mentally ill people living in nursing homes than any other state. In 2010, the state settled a class-action civil rights lawsuit, agreeing to help 5,000 of them transition into community programs within five years. As of July 2012, only 45 people had moved.
Nevada ($175.5 million in 2009 to $126.2 million in 2012, -28.1 percent): In 2003, Reno police calculated how much it cost the county to repeatedly pick up and hospitalize Murray Barr, a homeless man with an alcohol addiction. Tallying up doctors’ fees and other expenses from his decade on the streets, Barr racked up a $1 million bill.
District of Columbia ($212.4 million in 2009 to $161.6 million in 2012, -23.9 percent): Children on Medicaid wait 10 weeks—or one-third of the school year—for an appointment with a Children’s National Medical Center community clinic psychiatrist.
California ($3,612.8 million in 2009 to $2,848 million in 2012, -21.2 percent): Inmates with severe mental illness often wait three to six months for a state psychiatric hospital bed. In 2007, 19 percent of state prisoners were mentally ill. By 2012, 25 percent were.
crazy priorities
Approximately 10 percent of US homicides are committed by untreated severely mentally ill people.
Chances that a perpetrator of a mass shooting displayed signs of mental illness prior to the crime: 1 in 2
Between 1998 and 2006, the number of mentally ill people incarcerated in federal, state, and local prisons and jails more than quadrupled to 1,264,300.
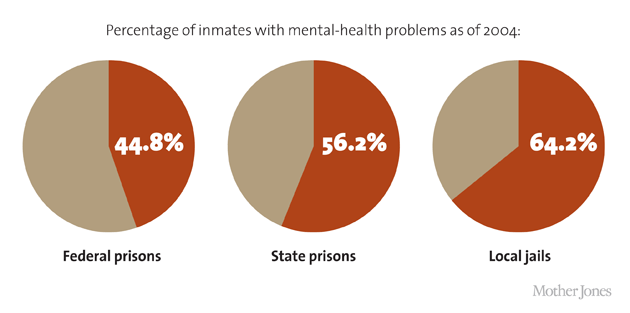
Since 2006, mental-illness rates in some county jails have increased by another 50 percent.
For every $2,000 to $3,000 per year spent on treating the mentally ill, $50,000 is saved on incarceration costs.
Prisoners with mental illness cost the nation an average of nearly $9 billion a year.
In 1955, there was one psychiatric bed for every 300 Americans. In 2010, there was one psychiatric bed for every 7,100 Americans—the same ratio as in 1850.
Severe mental disorders cost the nation $193.2 billion annually in lost earnings.

Sources for pie charts: National Coalition for the Homeless, NIMH, “Hunger and Homelessness Survey,” The US Conference of Mayors, “Inmate Mental Health,” National Institute of Mental Health
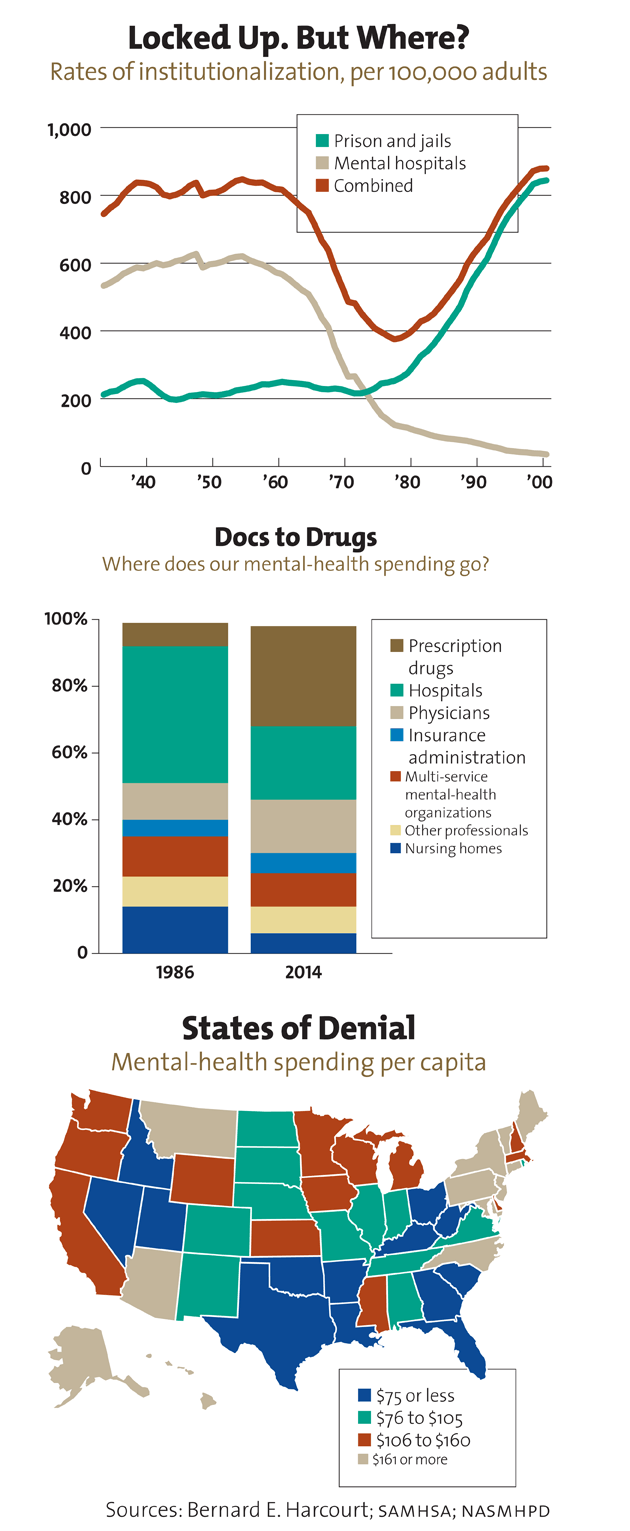
Source for “Locked Up. But Where”: Bernard Harcourt
Source for “Docs to Drugs”: US Dept. of Health and Human Services
Source for “States of Denial”: NRI